New Therapies for Atopic Dermatitis
Main article – scientific local news by NOC
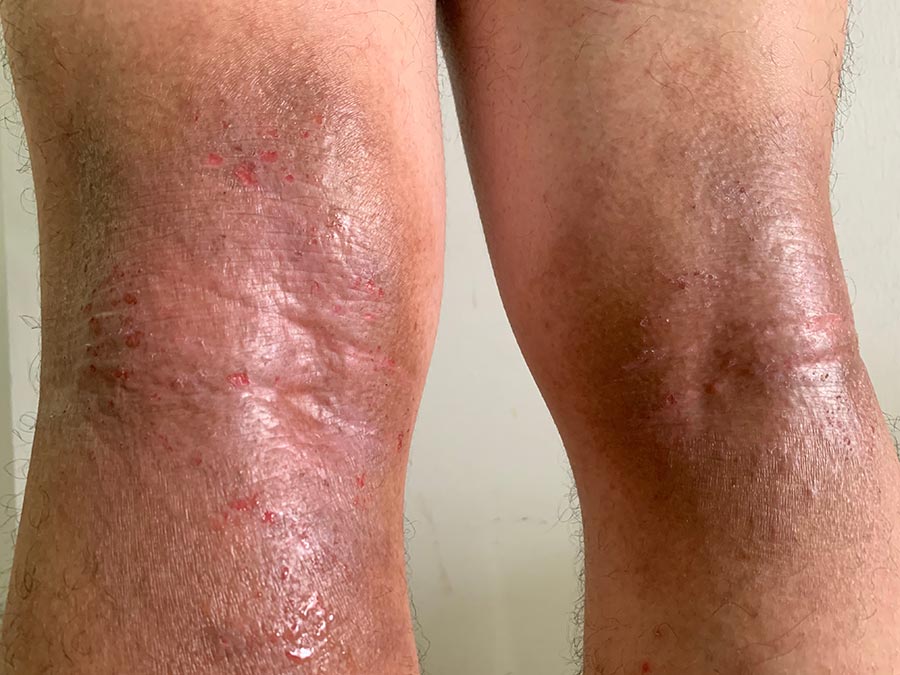
Over the last 2 decades, the understanding of the mechanism of atopic dermatitis has deepened significantly. The role of skin barrier dysfunction, immune dysregulation in the context of environmental triggers and genetic susceptibility has been further mapped out.
A/Prof LEE Haur Yueh,
President Dermatological Society of Singapore
Vice-President, 25th WCD Singapore
For a while, dermatologists have sat enviously on the sidelines as targeted therapies became routine treatments for other medical conditions. For the many patients with atopic dermatitis, topical treatments, phototherapy, traditional immunosuppressive agents were the only tools that we had. Globally, atopic dermatitis has the highest burden amongst skin disease; it affects up to 20% and 10% of children and adults respectively. The associated itch and skin pain is disabling, and many patients struggle with psychosocial issues and reduced quality of life. Over the last 2 decades, our understanding of the mechanism of atopic dermatitis has deepened significantly. The role of skin barrier dysfunction, immune dysregulation in the context of environmental triggers and genetic susceptibility has been further mapped out. These gains in our understanding have been translated to novel, state-of-the art treatments for our patients. These include novel biological therapies and small molecules targeting the JAK-STAT pathways.
Biological Therapies in Eczema
Anti IL-4/IL-13. Dupilumab was the first in-class, fully humanized monoclonal antibody (mAb) biologic that binds to IL4-Rα, a shared receptor for both IL-4 and IL-13. This was approved for moderate-to-severe atopic dermatitis in adults and pediatric patients age 6 years older. Since then, additional indications include moderate-to-severe eosinophilic asthma and chronic rhinosinusitis with nasal polyposis. Following the approval of Dupilumab, 2 other anti-IL13 monoclonal antibodies, Lebrikizumab and Tralokinumab are currently being evaluated.
Anti IL-31. The itch in atopic dermatitis is thought to be mediated by IL31. Nemolizumab, an IL-31 antibody was shown to improve pruritus, sleep as well as disease activity scores.
Anti TSLP. Thymic stromal lymphopoietin (TSLP) is a cytokine that drives type 2 inflammation, resulting in increased production of TH2 cytokines of IL-4, IL-5 and IL-13. Tezepelumab, a fully human monoclonal antibody is currently being evaluated.
Anti-OX 40. OX40-OX40 ligand binding potentiates and drives Th2 cell response. A humanized Ig G1 anti-OX40 mAb (GBR 830) Is undergoing evaluation
Other potential treatments may include agents antagonizing IL-22, IL17
Small Molecules
Janus Kinase (JAK) Inhibitors. These small oral molecules are promising therapies that target multiple downstream cytokines involved in AD through the inhibition of the JAK-STAT pathway. Baracitinib is a 1st generation oral JAK1/2 inhibitor that has been approved for moderate to severe AD in Europe and Japan. Similarly, Upadacitinib, a JAK1-selective inhibitor was also recently approved for treatment of moderate-to-severe atopic dermatitis in Europe. Abrocitinib, another oral, daily JAK1 selective inhibitor has also been granted marketing authorization in Europe. In addition to oral JAK inhibitors, various JAK inhibitors have been evaluated topically and are in different phases of development and approval. These include Tofacitinib (selective JAK 1/3 inhibitor), Ruxolitinib (selective JAK 1 & 2 inhibitor) as well as Delgocitinib (a pan-JAK inhibitor targeting JAK 1/2/3 and Tyk2).
With all these biologics and small molecules coming into the arena, new questions and challenges emerge; What is the long-term safety, efficacy and cost-effectiveness? How do we personalize treatment in such a heterogeneous, multi-faceted condition?
Without a doubt, many of these will be answered by the time the World Congress of Dermatology is held in Singapore.
Stay tuned. The wait is over, it is time to get in on the action!














